Introduction
If you’re suffering from severe temporomandibular joint (TMJ) disorder and surgery has been recommended, you’re likely facing two pressing concerns: finding relief and understanding the financial impact. The question of tmj surgery cost with insurance is complex because coverage varies dramatically between medical and dental plans, and insurers have strict criteria for what they consider medically necessary.
TMJ disorders affect the jaw joint and surrounding muscles, causing pain, clicking, popping, and limited jaw movement . When conservative treatments fail, surgery may become necessary—but these procedures can cost anywhere from $5,000 to over $50,000 depending on the type and complexity . Understanding how your insurance applies to these costs is essential for avoiding unexpected bills.
This guide covers five essential facts about tmj surgery cost with insurance, including how coverage works, what determines medical necessity, typical out-of-pocket expenses, and strategies to maximize your benefits.
Understanding TMJ Surgery Options and Their Costs
Before exploring tmj surgery cost with insurance, it’s important to understand the different surgical options available and their typical price ranges without coverage.
Types of TMJ Surgery
Why These Costs Vary
Several factors influence the final price of TMJ surgery:
- Surgeon expertise: Highly experienced, board-certified oral and maxillofacial surgeons typically charge higher fees
- Geographic location: Medical costs vary significantly by region, with urban areas generally more expensive
- Facility fees: Hospital stays cost more than outpatient surgical centers
- Anesthesia costs: Based on procedure type and duration
- Pre- and post-operative care: Consultations, imaging, medications, and follow-up appointments
The wide range of potential costs makes understanding tmj surgery cost with insurance crucial for financial planning.
Summary: Surgery Costs
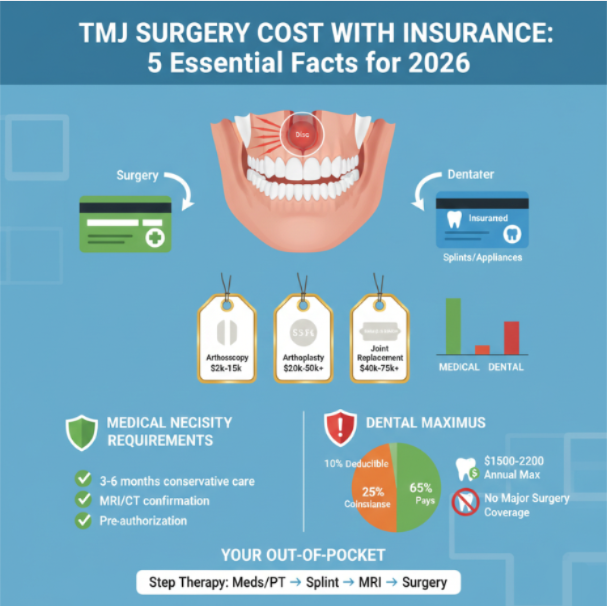
• Arthroscopy: $5,000-$15,000 (minimally invasive)
• Open joint surgery: $20,000-$50,000+
• Total joint replacement: $40,000-$50,000+
• Costs vary by surgeon, location, and facility type
Fact #1: Medical vs. Dental Insurance – Which One Covers TMJ Surgery?
One of the most confusing aspects of tmj surgery cost with insurance is determining whether your medical or dental plan provides coverage. The answer depends on how your condition is classified and the specific procedure.
Medical Insurance Coverage
TMJ surgery is often covered under medical insurance when it’s deemed medically necessary to treat a functional problem with the jaw joint . Major medical plans, including those from insurers like Aetna, typically cover surgical procedures when specific criteria are met .
Some group health benefit plans are required by state law to provide comparable coverage for medically necessary TMJ treatment as they do for other skeletal joints . This means that if your plan covers surgical treatment for other joints (like knees or hips), it must offer similar coverage for the temporomandibular joint.
Dental Insurance Coverage
Dental insurance plans may cover TMJ-related treatments, but often with different benefit structures. For example, some employer dental plans explicitly include “TMJ Services” as a covered category, typically paying 50% of costs after a deductible .
The Missouri State University dental plan for 2026 shows:
- TMJ Services (Class D): Paid at 50% after $50 deductible
- Annual maximum benefit: $3,000 per covered person
Cigna Dental Plans Example
Some dental plans, like the Cigna Dental PPO offered through certain benefit funds, include coverage for “TMJ Device and Adjustment” with specific cost-sharing:
Which Plan Applies?
The determination often comes down to:
Some insurance policies may require coordination between medical and dental plans, with each covering different aspects of treatment.
Summary: Insurance Type Matters
• Medical insurance typically covers surgical TMJ procedures deemed medically necessary
• Dental insurance often covers TMJ devices and adjustments at 50% coinsurance
• Some plans have annual maximums as low as $3,000 for all dental services
• Check both your medical and dental policies before proceeding
Fact #2: Medical Necessity Criteria Determine Coverage
Insurance companies don’t cover TMJ surgery automatically. They require proof that the procedure is medically necessary. Understanding these criteria helps you prepare for the approval process and anticipate tmj surgery cost with insurance.
Aetna’s Medical Necessity Requirements
Aetna’s Clinical Policy Bulletin for Temporomandibular Disorders outlines specific criteria for surgery coverage . TMJ surgery may be considered medically necessary when ALL the following general criteria are met:
- Conclusive evidence that severe pain or functional disability is produced by an intra-capsular condition
- Imaging confirmation of the intracapsular condition by MRI, computed tomography, or other imaging
- Failure of nonsurgical management – the condition has not responded to at least three months of conservative treatment, which may include:
Texas State Law Requirements
Texas law similarly requires that coverage be provided for medically necessary diagnosis or surgical treatment resulting from :
- Accident
- Trauma
- Congenital defect
- Developmental defect
- Pathology
What This Means for Your Coverage
Exceptions to Non-Surgical Management
In certain cases, immediate surgical intervention may be considered medically necessary without prior nonsurgical management, such as :
- Bony ankylosis (fusion of the joint)
- Failed TMJ total joint prosthetic implants
- Traumatic injury requiring urgent reconstruction
Summary: Medical Necessity Criteria
• Most insurers require 3-6 months of failed conservative treatment before approving surgery
• Imaging (MRI/CT) must confirm the joint condition
• Pre-authorization is typically required
• Some severe cases qualify for immediate surgical approval
Fact #3: What You’ll Actually Pay – Out-of-Pocket Costs with Insurance
Once your insurance approves TMJ surgery, your actual out-of-pocket expense depends on your specific plan’s cost-sharing structure. Understanding these components helps you estimate tmj surgery cost with insurance more accurately.
Cost-Sharing Components
Real-World Cost Examples
Example 1: Medical Insurance (Blue Cross Standard Option)
For a $30,000 TMJ arthroplasty with a surgeon in-network:
- Deductible (if not met): $500
- Coinsurance (15% of Plan allowance): ~$4,425
- Total out-of-pocket: ~$4,925
Calculation based on Blue Cross Standard Option paying 15% coinsurance after deductible
Example 2: Dental Insurance Only
For a $5,000 TMJ arthroscopy under dental insurance with 50% coinsurance:
- Deductible: $50
- Insurance pays 50% of $5,000 = $2,500
- Your coinsurance (50%): $2,500
- Total out-of-pocket: $2,550
Based on dental plan with $3,000 annual maximum and 50% coinsurance for TMJ services
Example 3: Medical + Dental Coordination
Some patients may have both medical and dental coverage that coordinate benefits. For example, medical might cover the surgical procedure while dental covers appliances or splints. Always check with both insurers about coordination of benefits.
The Annual Maximum Challenge
For dental plans, the annual maximum can significantly impact tmj surgery cost with insurance. Most dental plans cap benefits at $1,500-$3,000 per year . If your surgery costs $20,000 and your dental plan only pays up to $3,000 annually, you could be responsible for the remaining $17,000—plus your coinsurance.
Facility Fees and Anesthesia
Remember that your surgeon’s fee isn’t the only cost. Hospital or surgical center fees and anesthesia services are billed separately and subject to the same cost-sharing rules. Some plans have separate copayments based on where the procedure is performed .
Summary: Out-of-Pocket Costs
• Medical plans typically have deductibles ($500-$1,500+) and coinsurance (15-50%)
• Dental plans often pay 50% but have low annual maximums ($2,000-$3,000)
• Facility and anesthesia fees add significant costs
• Total out-of-pocket can range from a few thousand dollars to over $20,000 depending on coverage
Fact #4: The Pre-Authorization Process – Why It’s Critical
Failing to obtain proper pre-authorization is one of the biggest mistakes patients make when dealing with tmj surgery cost with insurance. Without it, you could be responsible for the entire bill.
When Pre-Authorization Is Required
Many insurers explicitly require pre-authorization for TMJ surgery. Aetna states that “requests for TMJ surgery require review by Aetna’s Oral and Maxillofacial Surgery patient management unit” . Blue Cross plans also note that “prior approval is required for oral/maxillofacial surgery needed to correct accidental injuries” .
What Pre-Authorization Involves
To obtain pre-authorization, your surgeon’s office typically submits:
Timeline Considerations
- Pre-authorization can take several weeks to process
- Some insurers have specific units dedicated to TMJ surgery review
- Emergency procedures within 72 hours of injury may have different rules
Consequences of Skipping Pre-Authorization
If you proceed without pre-authorization:
- Your claim may be denied entirely
- You could be responsible for 100% of costs
- Even if the procedure is eventually covered, penalties may apply
- Some providers require pre-authorization before they’ll schedule surgery
How to Verify Your Coverage
Before scheduling surgery:
- Call your insurance company with the specific procedure code (CPT code) your surgeon recommends
- Ask about pre-authorization requirements and obtain the necessary forms
- Request a pre-determination of benefits to get a written estimate of your out-of-pocket costs
- Confirm network status of your surgeon and facility
Summary: Pre-Authorization
• Most insurers require pre-authorization for TMJ surgery
• Documentation of failed conservative treatment is essential
• Processing can take weeks—plan ahead
• Skipping pre-authorization risks full financial responsibility
Fact #5: How to Appeal a Denied TMJ Surgery Claim
Even with strong medical necessity, TMJ surgery claims are sometimes denied. Understanding the appeals process can make the difference between paying out-of-pocket and getting coverage for tmj surgery cost with insurance.
Common Reasons for Denial
The Appeals Process
Step 1: Review the Denial Letter
Understand exactly why your claim was denied. The letter should cite specific policy language or criteria.
Step 2: Gather Additional Documentation
Work with your surgeon to collect:
- More detailed clinical notes
- Additional imaging or test results
- Letters supporting medical necessity
- Peer-reviewed literature supporting the procedure
Step 3: Submit a Formal Appeal
Follow your insurer’s appeals process, which typically involves:
- Written appeal letter addressing each reason for denial
- Supporting documentation
- Deadline compliance (usually 60-180 days from denial)
Step 4: External Review
If your internal appeal is denied, you may request an independent external review by a third party.
Tips for a Strong Appeal
- Involve your surgeon – A letter from your surgeon explaining why surgery is necessary carries significant weight
- Document everything – Keep copies of all submissions, correspondence, and deadlines
- Be persistent – Some patients succeed on second or third appeal
- Consider professional help – Patient advocates or attorneys specializing in insurance appeals can be valuable for complex cases
State Insurance Departments
If appeals are exhausted, contact your state insurance department. Some states have specific laws about TMJ coverage. For example, Texas law requires comparable coverage for TMJ as for other skeletal joints .
Summary: Appeals Process
• Understand exactly why your claim was denied
• Work with your surgeon to gather strong supporting documentation
• Follow formal appeals procedures and deadlines
• State insurance departments can help with unresolved disputes
What Insurance Companies Look for in TMJ Surgery Claims
Insurance companies have detailed criteria for evaluating TMJ surgery requests. Understanding what they’re looking for can help you prepare a stronger case for coverage of tmj surgery cost with insurance.
Aetna’s Procedure-Specific Criteria
Aetna’s policy outlines specific criteria for different surgical procedures :
| Procedure | Criteria for Coverage |
|---|---|
| Arthrocentesis | Imaging and clinical examination reveal anchored disc phenomenon, anterior disc displacement without reduction, osteoarthritis without fibrosis, open lock, or hemarthrosis |
| Therapeutic arthroscopy | MRI or other imaging confirms adhesions, fibrosis, degenerative joint disease, or internal derangement requiring modification |
| Arthroplasty/Arthrotomy | Imaging confirms osteoarthritis, severe disc displacement with degenerative changes, perforation, or severe scarring |
| Total joint replacement | End-stage disease with failed conservative and surgical management; imaging documents damaged condyles, recurrent ankylosis, or loss of condylar height |
The Importance of Comprehensive Documentation
Successful claims typically include:
- Detailed history – Onset, duration, progression of symptoms
- Physical examination findings – Range of motion, pain levels, joint sounds
- Imaging results – MRI, CT, or X-ray reports with specific findings
- Conservative treatment records – Dates, types, and outcomes of all nonsurgical therapies
- Functional impact – How the condition affects eating, speaking, and daily activities
The Role of the Specialist
Your oral and maxillofacial surgeon’s report is critical. It should clearly state:
- The specific diagnosis
- Why surgery is necessary
- How the procedure will address the underlying problem
- Why conservative treatments failed or were inappropriate
Summary: Insurer Criteria
• Each procedure type has specific coverage criteria
• Imaging must confirm the condition
• Failed conservative treatment must be documented
• Surgeon’s detailed report is essential
Frequently Asked Questions
1. Does insurance cover TMJ surgery?
It depends on your specific policy and whether the surgery is deemed medically necessary. Medical insurance may cover surgical TMJ procedures if criteria are met . Dental insurance often covers TMJ appliances at 50% coinsurance but has lower annual maximums .
2. How much is TMJ surgery with insurance out-of-pocket?
Out-of-pocket costs vary widely based on your plan. With medical insurance, you might pay 15-50% coinsurance after your deductible . With dental insurance, you typically pay 50% coinsurance up to your annual maximum ($2,000-$3,000) . Total costs can range from a few thousand dollars to over $20,000 depending on coverage.
3. What is the success rate of appealing a denied TMJ surgery claim?
Success rates vary, but strong documentation of medical necessity and failed conservative treatment significantly improves chances. Working closely with your surgeon and providing comprehensive records is essential.
4. How long does insurance pre-authorization for TMJ surgery take?
Pre-authorization typically takes 2-4 weeks, but can take longer if additional information is requested. Some insurers have specialized review units for TMJ surgery . Plan ahead and submit all required documentation promptly.
5. Does Medicare cover TMJ surgery?
Medicare coverage for TMJ surgery varies by plan and medical necessity. Check with your specific Medicare Advantage or supplemental plan for details. Some TMJ surgical procedures have specific Medicare Benefits Schedule items in other countries .
6. Can I use both medical and dental insurance for TMJ surgery?
Possibly. Some patients have coordination of benefits where medical covers surgery and dental covers appliances. Check with both insurers about their coordination policies and provide documentation to both.
7. What if my TMJ surgery is denied as “not medically necessary”?
You have the right to appeal. Work with your surgeon to gather additional documentation showing failed conservative treatment and objective imaging findings . Consider an independent external review if internal appeals are denied.
8. Does insurance cover TMJ splints or oral appliances?
Dental insurance often covers TMJ devices at 50% coinsurance . Medical insurance may cover them as part of nonsurgical management, but policies vary. Check your specific plan documents.
9. How do I find a TMJ surgeon who accepts my insurance?
Contact your insurance company for a list of in-network oral and maxillofacial surgeons. Verify network status before scheduling, as some providers may be in-network for dental but not medical procedures .
10. What questions should I ask my insurance company about TMJ surgery coverage?
Ask about: pre-authorization requirements, deductible and coinsurance amounts, annual maximums, network status of your surgeon, documentation needed, and appeals process if denied.
Summary: TMJ Surgery Cost with Insurance
Understanding tmj surgery cost with insurance requires navigating complex coverage rules, medical necessity criteria, and cost-sharing structures. Here are the key takeaways:
Key Takeaways
- Surgery costs are significant: TMJ surgery ranges from $5,000 to over $50,000 without insurance, depending on procedure type and complexity .
- Medical vs. dental insurance: Surgical TMJ procedures are typically covered under medical insurance when medically necessary , while dental plans often cover appliances at 50% coinsurance with low annual maximums .
- Medical necessity is key: Insurers require 3-6 months of failed conservative treatment, imaging confirmation of joint pathology, and pre-authorization .
- Out-of-pocket costs vary: With medical insurance, you might pay 15-50% coinsurance after deductible . With dental insurance, you typically pay 50% up to a $2,000-$3,000 annual maximum .
- Pre-authorization is critical: Most insurers require advance approval. Skipping this step risks full financial responsibility .
- Appeals are possible: If denied, work with your surgeon to gather strong documentation and follow formal appeals procedures. State insurance departments can help .
- Document everything: Comprehensive records of conservative treatment, imaging, and surgeon recommendations are essential for coverage .
The most important takeaway? Don’t assume your TMJ surgery will be covered—verify coverage, obtain pre-authorization, and document medical necessity thoroughly. A proactive approach to understanding tmj surgery cost with insurance can save you thousands of dollars and prevent unexpected bills.
Work closely with your oral and maxillofacial surgeon’s office—they handle insurance pre-authorizations regularly and can guide you through the process. Schedule a consultation, request a detailed cost estimate, and contact your insurance company with specific questions about your policy’s TMJ coverage.
Conclusion
The question of tmj surgery cost with insurance doesn’t have a simple answer—it depends on your specific policy, the type of surgery recommended, and whether you meet medical necessity criteria. What’s clear is that TMJ surgery represents a significant financial investment, with procedures ranging from $5,000 to well over $50,000 .
Insurance coverage for TMJ surgery follows a distinct pattern: medical insurance typically covers surgical procedures when they’re deemed medically necessary to treat an intracapsular condition , while dental insurance often covers TMJ appliances and devices at 50% coinsurance but with lower annual maximums . Some group health plans are required by state law to provide comparable coverage for TMJ as for other skeletal joints .
The path to coverage requires several critical steps:
- Document conservative treatment – Most insurers require proof that you’ve tried at least 3-6 months of nonsurgical management
- Obtain objective imaging – MRI or CT confirmation of joint pathology is essential
- Secure pre-authorization – Submit all documentation to your insurer before scheduling surgery
- Verify network status – Confirm your surgeon and facility are in-network
- Understand your out-of-pocket costs – Review your plan’s deductible, coinsurance, and annual maximums
If your claim is denied, don’t give up. Work with your surgeon to gather additional supporting documentation and file a formal appeal. Some patients succeed on second or third appeal, and state insurance departments can help with unresolved disputes .
Your journey to TMJ relief shouldn’t be derailed by insurance confusion. Take these steps today:
- Call your insurance company to request a copy of your policy’s TMJ coverage criteria
- Schedule a consultation with a board-certified oral and maxillofacial surgeon
- Ask the surgeon’s office about their experience with insurance pre-authorization
- Begin documenting any conservative treatments you’ve tried
With careful planning and thorough documentation, you can navigate the complexities of tmj surgery cost with insurance and focus on what really matters: finding relief from TMJ pain and restoring your quality of life.
References
- Equity League Benefit Funds. (2026). Dental Plans – Cigna Coverage.
- Texas Department of Insurance. (1997). Commissioner’s Bulletin – HB 2063: Diagnosis and Treatment of Conditions Affecting the Temporomandibular Joint (TMJ).
- Advance Study. (2025). How Much Does TMJ Reduction Cost by Surgeon?
- Blue Cross and Blue Shield Service Benefit Plan. (2026). FEHB Standard and Basic Options – Oral and Maxillofacial Surgery.
- Aetna. (2026). Clinical Policy Bulletin: Temporomandibular Disorders (Number: 0028).
- Missouri State University. (2026). Dental Insurance – 2026 Rates and Coverage.
- WeCovr. (2026). Does Insurance Cover Private TMJ Jaw Maxillofacial Surgery?
- Australian Government Department of Health. (2025). Medicare Benefits Schedule – Item 45857 (TMJ Arthroscopy).
- Australian Government Department of Health. (2025). Medicare Benefits Schedule – Item 53226 (TMJ Synovectomy).
Disclaimer:
The content provided is for informational purposes only and does not constitute medical or insurance advice. While efforts are made to ensure accuracy, no guarantees are given regarding completeness or reliability. Insurance policies, coverage criteria, and costs vary by provider, plan, and individual circumstances. Any action you take upon the information is strictly at your own risk. We recommend consulting directly with your insurance provider and healthcare professionals for advice regarding your specific situation.